Trust is the foundation of quality care. When patients don’t trust their providers, they hesitate to seek guidance, question medical advice, or delay critical treatments. When care teams don’t trust their own systems, inefficiencies compound, handoffs break down, and outcomes suffer.
Imagine a patient being discharged from a hospital, only to arrive at a skilled nursing facility that wasn’t expecting them, lacks the resources to care for them, or—worse—refuses to accept them altogether. It’s a breakdown in communication, but at its core, it’s a breakdown in trust. Care managers, post-acute providers, and payers must work together to ensure that every patient transition is smooth, timely, and centered on the patient’s well-being.
CM Converge—an annual care management thought leadership retreat hosted by Aidin— brought together changemakers in healthcare in 2025 to discuss the intersection of technology, trust, and innovation in care management. From strategic incentives to technology-driven efficiencies, interactive sessions explored how health systems nationwide can streamline care management workflows, improve collaboration, and build more trust between patients and providers.
Below are seven key takeaways from the conference:
1. Trust drives influence in healthcare
Leaders emphasized that trust in healthcare is earned through transparency, consistency, and accountability.
During one panel, AdventHealth’s Corporate Executive Director of Care Management, Jeannine Nylaan, shared insights on how their organization’s “bowtie model” ensures that system-wide decisions align with frontline care needs. This strategy prioritizes executive buy-in by proving that market-level demands originate from tangible provider needs.
One critical component Jeannine highlighted in discussions with other panelists was the importance of visibility at all levels of care management. Decision-makers must engage with frontline staff, ensuring that their strategies reflect real-world challenges. By creating a model where regional leaders participate in decision-making, AdventHealth ensures that changes in processes or technology are practical across their 50+ hospital system, not just theoretical.
Additionally, panelists discussed how storytelling plays a vital role in gaining executive buy-in. Sharing real-life examples of care improvement—whether reducing unnecessary admissions or improving discharge planning—helps leaders understand the tangible impact of their initiatives. Trust is built when executives see the direct correlation between policy decisions and patient outcomes.
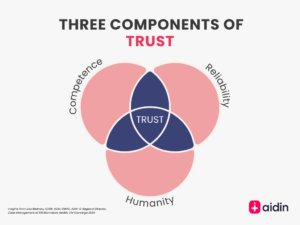
2. The trust equation: Competence, reliability, and humanity
Lisa Bednarz, LCSW, ACM, CMAC, ASW-G, Regional Director, Case Management at RWJBarnabas Health, broke down trust in healthcare into a measurable equation:
- Competence: Clinicians must stay informed and communicate clearly.
- Reliability: Healthcare teams must set clear expectations and meet them.
- Humanity: Empathy in patient interactions fosters confidence.
This equation helps guide organizations in addressing patient skepticism and strengthening long-term relationships. Lisa emphasized that trust is not just a patient issue—it’s an operational one. When frontline staff lacks trust in leadership, adoption of new initiatives slows, and the quality of care can be negatively impacted.
One example highlighted was the role of case managers in trust-building. Patients often find it difficult to navigate post-acute care options, which can lead to frustration and non-compliance. Case managers who proactively educate patients on their options—and consistently follow up—can improve outcomes significantly. Providing patients with clear, accurate expectations reduces anxiety and fosters trust in the system.
3. Connecting care through trust
Presenters also shared how trust plays a crucial role in ensuring smooth patient transitions. They emphasized that successful post-acute partnerships must be built on accountability and transparency.
Dr. Ada Offurum, Assistant Dean for Faculty Affairs and Professional Development at the University of Maryland School of Medicine, described the challenge of securing placements for vulnerable patients—particularly those with complex medical needs and challenging payer mixes. Establishing direct, reliable relationships with skilled nursing facilities and home care agencies has been critical in ensuring that individuals aren’t left without options. Trust, in this context, means ensuring that when a post-acute provider commits to taking a patient, they follow through.
Stacy Galik, Director of Hospital Care Coordination, West Region, BayCare Health System, highlighted how her organization has improved care transitions by developing strong community partnerships—including collaborations with the Salvation Army and Feeding Tampa Bay. By addressing social determinants of health (SDoH)—such as food insecurity—BayCare has strengthened patient confidence in the healthcare system, showing that connected and compassionate care can extend beyond hospital walls.
One of the most significant advancements Stacy discussed was BayCare’s new approach to skilled nursing facility authorizations. By taking control of the authorization process through Aidin’s care management platform, BayCare reduced delays and improved patient placement efficiency. The ability to manage authorizations internally has eliminated opportunities for facilities to stall or misrepresent approval timelines, leading to faster discharges and better patient outcomes.
Ready to learn more about how BayCare leveraged Aidin to improve care management? Download our eBook for more insights.
4. Technology as a trust multiplier
Aidin CEO Russ Graney highlighted how technology can reinforce trust in healthcare by establishing clear rules and accountability. Aidin’s platform offers features like provider badges and automated response deadlines to help maintain integrity while streamlining care transitions.
Russ’s analogy illustrated how technology can take on the role of the “honest broker” in healthcare. A key challenge in care transitions is the variability in responsiveness from post-acute providers. By setting clear benchmarks and rewarding those who adhere to deadlines—such as response times for referrals—Aidin ensures that care managers receive consistent, timely data. This consistency builds trust across the system.
Another takeaway was the importance of user experience in healthcare software. Adoption rates suffer if a platform is difficult to navigate or adds an administrative burden. Aidin’s success is largely attributed to its intuitive interface, which simplifies workflow instead of complicating it.
5. Aligning incentives to build a sustainable system
Ronald Hirsch, MD, Vice President, Physician Advisory Solutions at R1 RCM & Advisory Board Member with American College of Physician Advisors, spoke on the need to realign incentives so that patient outcomes—not administrative burdens—dictate decision-making. He challenged hospital leaders to ensure that financial structures support quality care rather than unintentionally rewarding inefficiencies.
A crucial takeaway was that misaligned incentives can erode trust. When patients feel they are receiving unnecessary care—or being discharged too soon due to cost concerns—they lose confidence in the system. Hospitals can improve trust and operational efficiency by aligning financial incentives with patient-centered care.
6. The role of case managers in rebuilding patient confidence
Case managers serve as the bridge between healthcare systems and real-world patient experiences. Tiffany Ferguson, CEO of Phoenix Medical Management, emphasized the growing compliance expectations surrounding social determinants of health (SDoH) and how proactive case management can prevent avoidable readmissions.
One emerging challenge is that trust in healthcare has declined due to inconsistencies in patient experience. Individuals may receive different information from different care providers, leading to confusion and skepticism. Tiffany stressed the importance of standardized communication across case management teams.
She also highlighted the role of social determinants of health in trust-building. Patients facing housing insecurity, food instability, or lack of transportation are at higher risk for poor outcomes. Hospitals that actively address these barriers—by collaborating with community organizations and payers—can significantly improve patient trust and long-term health outcomes.
Change is hard—but necessary for building trust
Throughout CM Converge’s vibrant discussions, a recurring theme emerged time and time again: the challenge of unlearning outdated processes. Whether adopting new referral technology or shifting patient discharge strategies, leaders agreed that change requires both patience and persistence.
The panelists acknowledged that resistance to change is natural but must be addressed through transparency and consistent reinforcement of long-term benefits. Our annual care management conference reinforced a simple truth: trust isn’t automatic—it’s built through transparency, reliability, and the right use of technology. And organizations that prioritize these principles will be best positioned to navigate the future of care management.
Want to learn more about how Aidin is building trust through smarter care management? Get in touch today.
About the author
Lindsey North is the Senior Director of Client Experience at Aidin, where she leads implementation and client success efforts with deep expertise in care management transformation. She brings over 15 years of healthcare experience, including leadership of hospital care coordination across ten acute care hospitals at BayCare Health System. Lindsey has been a trusted voice in the field, designing training programs that empower care teams. She is passionate about driving positive change in patient care and guiding teams through effective change management.

